Diabetes & The Eye

Diabetes is a condition which can affect many systems in the body. It occurs when the level of sugar (glucose) in our blood is higher than normal. There are two main types of diabetes: type 1 and type 2. Type 1 diabetes is autoimmune, meaning the immune system of your body attacks its own cells in the pancreas that control levels of blood glucose.1 Type 2 diabetes is a progressive condition where the body becomes resistant to the effects of and/or slowly produces less of the glucose-controlling hormone,insulin.1 Both type 1 and type 2 diabetes can cause changes to the tissues and blood vessels at the front and back of the eye after a period of time.1 All diabetics should ensure they visit their optometrist at least annually for a thorough examination.

Diabetic retinopathy
Diabetic retinopathy (DR) is a condition where high blood sugar levels damage the small blood vessels (or capillaries) in the back of your eye, also known as the retina. The risk of developing these changes increases the longer you have had diabetes and the less controlled itis. There are two major categories of diabetic retinopathy:
- Non-proliferative: The capillaries in the retina become weak, leading to small bulges in the vessel wall (microaneurysms) and other vessel wall changes, causing reduced blood circulation in the retina.3
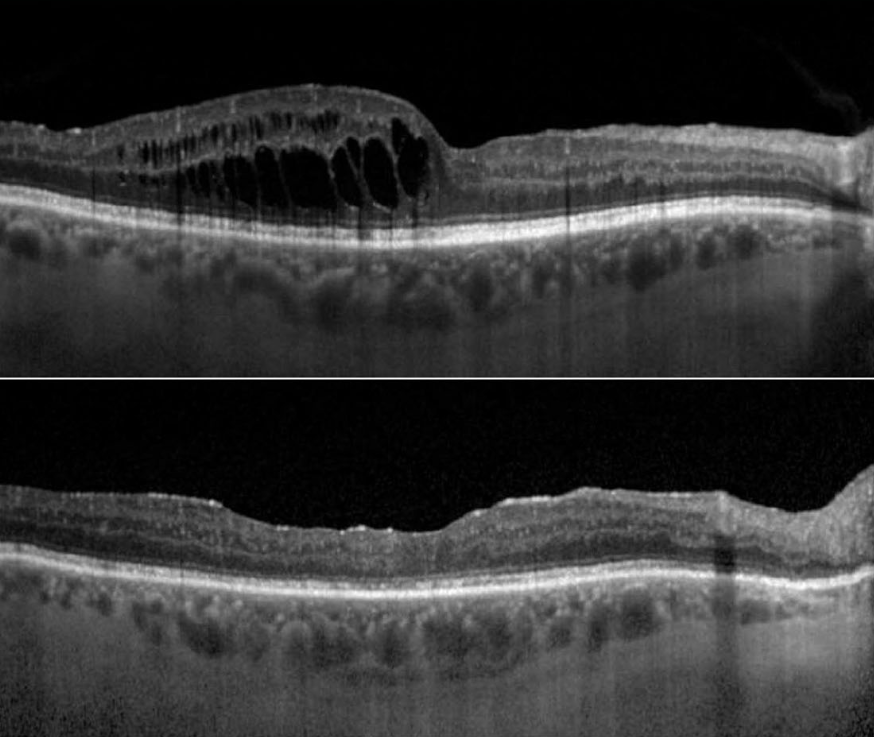
- Proliferative: Damage to vessels becomes so severe that the retina is significantly starved of oxygen, leading to the creation of new, leaky vessels to compensate which can cause extensive bleeding and sudden vision loss.3
INSERT IMAGE
Other complications of diabetes
Cataract: The lens at the front of the eye becomes clouded with reduced oxygen delivery.4
Changing focussing ability: Focus may weaken or fluctuate from day to day due to swelling of the lens.4 This has often led to the diagnosis of diabetes in many cases. The problem eases when blood glucose levels are well controlled.
Blurred or ‘greyed-out’ vision: Fluid build-up in the back of the eye with leakage of blood vessels near the very centre of vision, known as diabetic macular oedema, prevents light from being effectively transmitted.3
Double vision: This is a distressing but rare complication of diabetes.4 The condition is usually temporary, but it may last for a few months. An optometrist can help to treat it while it has effect. Diabetes is not the only cause of double vision, so it is best to have this checked by your optometrist if it occurs.
Dry eyes: Most cases of diabetic dry eye arise when the nerves that supply the tear gland (Lacrima gland) become damaged.4 This is the same process that causes symptoms like tingling or burning in the hands and feet, can also affect the nerves that normally sense dryness of the eye and signal for more tear production. See our dry eye page for more information here.
Diabetic care at Innovative Eye Care
Controlling blood glucose over time significantly reduces the risk of developing retinopathy but does not eliminate it. Routine eye examinations are the best management to prevent or detect diabetes-related complications sooner rather than later.
Our optometrists will often use eye drops to increase your pupil size (dilating drops), allowing for a better view into the back of the eye. A good analogy is like looking through a keyhole compared to opening up the door. A full dilated retinal examination is recommended at least once a year to monitor for retinal signs of diabetes, which are often stealthy and change without your knowledge. Dilating drops last for 4-6 hours and can cause glare and blurry vision, so we recommend waiting for a short period before driving.
With the aid of our Heidelberg OCT, we are able to detect signs of diabetic retinopathy and diabetic macular oedema in all stages of the conditions. With the addition of OCT-A imaging, we can perform non-invasive 3D scans of the blood vessel network in the eye. Monitoring the movement of individual blood cells allows for greater analysis of diabetic eye health. We also have specialised equipment to help detect and manage cataracts and dry eye disease, including corneal tomography and topography, slit lamp biomicroscope and anterior eye imaging.
The role of optometry in diabetic management is that of close monitoring and communication with other health professionals involved in your diabetic care. If we detect the development of diabetic retinopathy, we can alter diabetic control and management with the help of your GP, endocrinologist and ophthalmologist.
References
1) Sapra A, Bhandari P. Diabetes Mellitus.In:StatPearls [Internet]. Treasure Island (FL):StatPearlsPublishing; 2020[cited 2020 Nov 19]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK551501/
2) Diabetes Australia. Diabetes in Australia[Internet]. n.d. [cited 2020 Nov 19]. Available from: https://www.diabetesaustralia.com.au/about-diabetes/diabetes-in-australia/
3) Fraser CE, D’Amico DJ. Diabetic retinopathy: Prevention and treatment [Internet]. 2014 [cited 2016 Oct 14].Available from: https://www.uptodate.com/contents/diabetic-retinopathy-prevention-and-treatment?source=see_link
4) Sayin N, Kara N, Pekel G. Ocular complications of diabetes mellitus. World J Diabetes. 2015 Feb 15;6(1):92–108.
FAQs
Please browse through some of our most frequently asked questions on this topic.
Speak to our friendly team today
Book your appointment now for personalised eye care tailored just for you.









